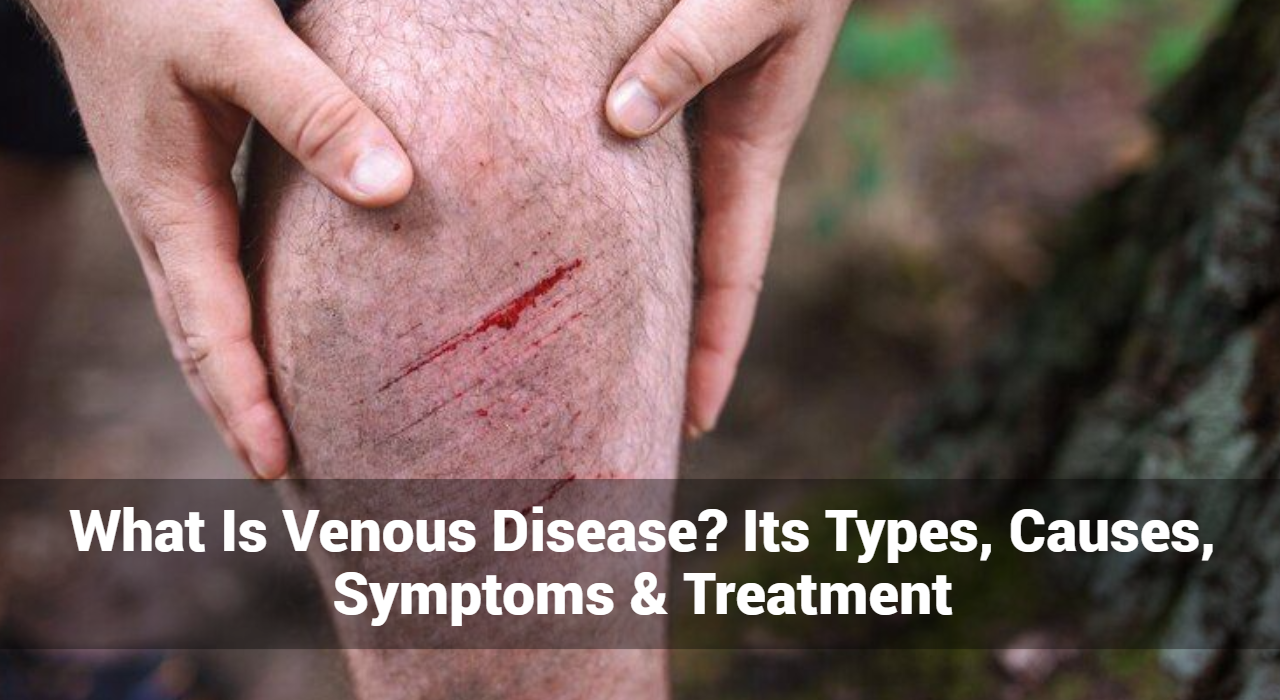
Venous disease, also known as venous insufficiency, is a condition in which the veins in the body do not properly return blood to the heart. This can lead to a range of symptoms and complications, from mild discomfort to severe health issues. Understanding the types, causes, symptoms, and treatment options for venous disease is crucial for effective management and prevention.
What is Venous Disease?
Venous disease occurs when veins become damaged or dysfunctional, affecting their ability to transport blood efficiently. This condition can affect any veins in the body, but it most commonly impacts those in the legs. Veins have one-way valves that prevent blood from flowing backward. When these valves fail, blood can pool in the veins, leading to various complications.
Common Types of Venous Disease
- Varicose Veins
- Description: Enlarged, twisted veins that are often visible under the skin.
- Symptoms: Aching, swelling, and a feeling of heaviness in the legs. They may also cause itching and skin discoloration.
- Spider Veins
- Description: Small, red, blue, or purple veins that appear close to the surface of the skin.
- Symptoms: Typically asymptomatic but can cause cosmetic concerns and mild discomfort.
- Chronic Venous Insufficiency (CVI)
- Description: A long-term condition where the veins cannot pump enough blood back to the heart.
- Symptoms: Swelling, skin changes, and ulcers on the legs.
- Deep Vein Thrombosis (DVT)
- Description: A blood clot that forms in a deep vein, usually in the legs.
- Symptoms: Swelling, pain, and redness in the affected leg. DVT can lead to serious complications if the clot travels to the lungs (pulmonary embolism).
- Superficial Thrombophlebitis
- Description: Inflammation and clotting in a superficial vein.
- Symptoms: Redness, swelling, and pain along the affected vein.
What Causes of Venous Disease?
01. Genetics
- A family history of venous disease increases the risk of developing the condition.
02. Age
- The risk of venous disease increases with age due to the weakening of vein walls and valves over time.
03. Gender
- Women are more likely to develop venous disease, partly due to hormonal changes related to pregnancy, menopause, and the use of birth control pills.
04. Prolonged Standing or Sitting
- Jobs that require long periods of standing or sitting can contribute to venous disease by hindering blood flow.
05. Obesity
- Excess weight puts additional pressure on veins, increasing the risk of venous disease.
06. Pregnancy
- Pregnancy increases blood volume and puts additional pressure on veins, leading to an increased risk of venous disease.
07. Injury or Surgery
- Damage to veins from injury or surgery can lead to venous insufficiency.
08. Lack of Exercise
- Regular exercise helps maintain healthy blood flow. A sedentary lifestyle can contribute to venous disease.
Track and Manage your Eczema treatment using a comprehensive Eczema App
Download Eczemaless now
What Are The Symptoms of Venous Disease?
1. Swelling
- Typically in the legs and ankles, swelling is a common symptom of venous disease.
2. Pain and Discomfort
- Aching, throbbing, or a feeling of heaviness in the legs.
3. Skin Changes
- Discoloration, dryness, or the development of ulcers, particularly around the ankles.
4. Visible Veins
- Enlarged, twisted, or bulging veins (varicose veins) and small, web-like veins (spider veins).
5. Itching and Burning
- A sensation of itching or burning in the affected areas.
6. Leg Cramps
- Particularly at night, leg cramps can be a symptom of venous disease.
7. Restless Legs
- A compelling urge to move the legs, often accompanied by uncomfortable sensations.
Diagnosis of Venous Disease
Diagnosing venous disease typically involves a physical examination and medical history review. Additional diagnostic tests may include:
- Duplex Ultrasound
- This non-invasive test uses sound waves to visualize blood flow in the veins and detect clots or blockages.
- Venography
- A special dye is injected into the veins, and X-rays are taken to visualize the veins and identify any abnormalities.
- Magnetic Resonance Venography (MRV)
- An MRI scan that provides detailed images of the veins.
What Are The Treatment Options for Venous Disease?
1. Lifestyle Changes
- Exercise: Regular physical activity helps improve blood flow and strengthen the calf muscles, which play a crucial role in venous return.
- Diet: Maintaining a healthy weight and eating a balanced diet can reduce pressure on the veins.
- Elevating the Legs: Elevating the legs above the heart level can help reduce swelling and improve blood flow.
2. Compression Therapy
- Compression Stockings: Specially designed stockings apply pressure to the legs, helping veins move blood more efficiently. They come in different levels of compression and lengths.
3. Medications
- Blood Thinners: Used to treat and prevent blood clots in conditions like DVT.
- Anti-inflammatory Medications: Help reduce pain and swelling associated with venous disease.
4. Minimally Invasive Procedures
- Sclerotherapy: A solution is injected into the affected veins, causing them to collapse and eventually be absorbed by the body.
- Endovenous Laser Treatment (EVLT): A laser fiber is inserted into the vein, emitting energy that causes the vein to collapse.
- Radiofrequency Ablation (RFA): Similar to EVLT, this procedure uses radiofrequency energy to heat and close off the vein.
5. Surgical Treatments
- Vein Stripping: Removal of the affected vein through small incisions.
- Ambulatory Phlebectomy: Removal of varicose veins through tiny punctures in the skin.
- Vein Bypass: Creating a bypass around the damaged vein using a healthy vein from another part of the body.
How Can Prevent of Venous Disease
1. Stay Active
- Regular exercise, such as walking, swimming, or cycling, promotes healthy blood flow.
2. Maintain a Healthy Weight
- Keeping a healthy weight reduces pressure on the veins.
3. Avoid Prolonged Standing or Sitting
- Take breaks to walk around or stretch if your job requires long periods of sitting or standing.
4. Elevate Your Legs
- Elevate your legs when resting to help reduce swelling and improve circulation.
5. Wear Compression Stockings
- Compression stockings can help prevent venous disease, especially if you are at high risk.
6. Stay Hydrated
- Drinking plenty of water helps maintain healthy blood circulation.
GET IN CONTROL OF YOUR ECZEMA
Use our AI tool to check the severity of Eczema and keep track of your Eczema progress.
Home Remedies for Venous Disease
Venous disease, which encompasses conditions such as varicose veins, spider veins, and chronic venous insufficiency, can be managed effectively with lifestyle changes and home remedies. While medical treatments are often necessary, incorporating home remedies can provide relief from symptoms and improve overall vascular health. Here are some effective home remedies for venous disease.
1. Compression Stockings
How They Help: Compression stockings apply pressure to the legs, helping veins move blood more efficiently back to the heart. They can reduce swelling, discomfort, and the risk of developing further venous complications.
Usage:
- Wear compression stockings as directed by your healthcare provider, usually throughout the day.
- Ensure they fit properly to avoid discomfort or skin damage.
2. Elevate Your Legs
How It Helps: Elevating your legs above heart level helps reduce swelling and improves blood flow by using gravity to assist venous return.
Usage:
- Lie down and prop your legs on pillows or a cushion.
- Elevate your legs for 15-30 minutes several times a day.
3. Regular Exercise
How It Helps: Exercise promotes healthy blood circulation and strengthens the calf muscles, which play a crucial role in pushing blood back to the heart.
Suggestions:
- Engage in low-impact activities such as walking, swimming, or cycling.
- Aim for at least 30 minutes of exercise most days of the week.
4. Maintain a Healthy Weight
How It Helps: Excess weight puts additional pressure on veins, exacerbating venous disease symptoms.
Tips:
- Follow a balanced diet rich in fruits, vegetables, lean proteins, and whole grains.
- Monitor portion sizes and avoid high-calorie, low-nutrient foods.
5. Herbal Remedies
a. Horse Chestnut Extract:
- How It Helps: Horse chestnut contains aescin, which helps improve venous tone and reduce swelling.
- Usage: Available in supplement form or topical creams. Consult with a healthcare provider for proper dosage.
b. Grape Seed Extract:
- How It Helps: Rich in antioxidants, grape seed extract can help strengthen blood vessels and reduce inflammation.
- Usage: Take as a supplement, following the recommended dosage on the packaging.
c. Gotu Kola:
- How It Helps: Gotu kola may improve circulation and reduce swelling.
- Usage: Available as a supplement or in topical creams. Follow dosage recommendations.
6. Dietary Changes
How It Helps: A diet rich in certain nutrients can support vein health and reduce symptoms of venous disease.
Recommendations:
- Fiber: Prevents constipation, reducing pressure on veins. Include foods like whole grains, fruits, and vegetables.
- Flavonoids: Strengthen blood vessels and improve circulation. Found in foods like berries, citrus fruits, and dark chocolate.
- Vitamin C: Supports collagen production, essential for vein health. Include citrus fruits, strawberries, and bell peppers.
- Vitamin E: Improves blood flow. Found in nuts, seeds, and leafy greens.
7. Hydration
How It Helps: Staying hydrated helps maintain healthy blood circulation and prevents blood from becoming too thick.
Tips:
- Drink plenty of water throughout the day.
- Limit intake of dehydrating beverages like alcohol and caffeine.
8. Avoid Prolonged Sitting or Standing
How It Helps: Prolonged periods of sitting or standing can hinder blood flow and exacerbate venous disease symptoms.
Tips:
- Take breaks to walk around or stretch every hour if you have a sedentary job.
- Shift your weight and move your legs regularly if you must stand for long periods.
9. Wear Loose Clothing
How It Helps: Tight clothing, especially around the waist and legs, can restrict blood flow and worsen venous disease.
Tips:
- Opt for loose-fitting, comfortable clothing.
- Avoid tight belts, leggings, or stockings that aren’t designed for compression therapy.
10. Massage
How It Helps: Gentle massage can help improve circulation and reduce swelling in the legs.
Tips:
- Use upward strokes, starting from the ankles and moving towards the heart.
- Use a moisturizing lotion or oil to reduce friction and improve comfort.
11. Essential Oils
How They Help: Certain essential oils can promote circulation and reduce swelling.
Suggestions:
- Cypress Oil: Known for its circulation-boosting properties. Dilute with a carrier oil and massage into the affected area.
- Lavender Oil: Provides relief from pain and inflammation. Dilute and apply as needed.
- Peppermint Oil: Offers a cooling effect and helps reduce swelling. Dilute before use.
12. Hydrotherapy
How It Helps: Alternating between hot and cold water can improve circulation and reduce swelling.
Usage:
- End your shower with a blast of cold water on your legs.
- Use warm water for a few minutes, followed by cold water for a minute. Repeat this cycle several times.
Conclusion
Venous disease is a common skin condition that can significantly impact quality of life if left untreated. By understanding the types, causes, symptoms, and available treatments, individuals can take proactive steps to manage and prevent venous disease. If you suspect you have venous disease, it is essential to consult with a healthcare provider for an accurate diagnosis and appropriate treatment plan. With proper management, many people with venous disease can lead healthy, active lives.
Track and Manage your Eczema treatment using a comprehensive Eczema App
Download Eczemaless now