Got itchy skin? It might be Eczema

- Introduction
- What is Eczema?
- What are the signs and symptoms of Eczema?
- Why does Eczema itch?
- Does Eczema run in families?
- What are the causes of Eczema?
- Can you manage your Eczema?
- Over the Counter products for Eczema?
- When should you seek help?
Introduction
Does your itch skin and become inflamed from time to time? Does it itch so bad that you feel like scratching it until your skin is damaged? This might be eczema.
Eczema is also called atopic dermatitis, which is commonly seen in children, but it can occur in adults too. Eczema can be controlled well if you seek medical attention. Unfortunately it is not curable, as it recurs from time to time even after complete remission.
What is Eczema?
Track and Manage your Eczema treatment using a comprehensive Eczema App
Download Eczemaless now


Eczema derives from the Greek word “boil”. It accounts for a large proportion of skin disease in the developed as well as the developing world. It is estimated that Eczema affects about 16.5 million adults and more than 9.6 million children in USA. Up to 40% of the population may suffer from eczema during their life time and at any given time, about 10% of the population may have some form of eczema. It can have a vast impact on the quality of life of an individual who suffers from eczema, if it is not properly controlled.
Eczema is a chronic skin condition which may have several flares and remissions. In most eczema patients there are periods when the skin condition is worse, which is called a flare or exacerbation. It is followed by periods of skin improvements or entire clear up which is known as remission.
Eczema usually begins between of 2 -3 months of age. It commonly starts during childhood and continues in to adulthood. Some individuals may go in to total remission during their teenage years. Although eczema usually starts in childhood, adults may get it for the first time which is known as adult onset eczema.
The good news is that Eczema is not contagious and you cannot spread it to someone by touch. It is not associated with poor hygiene.
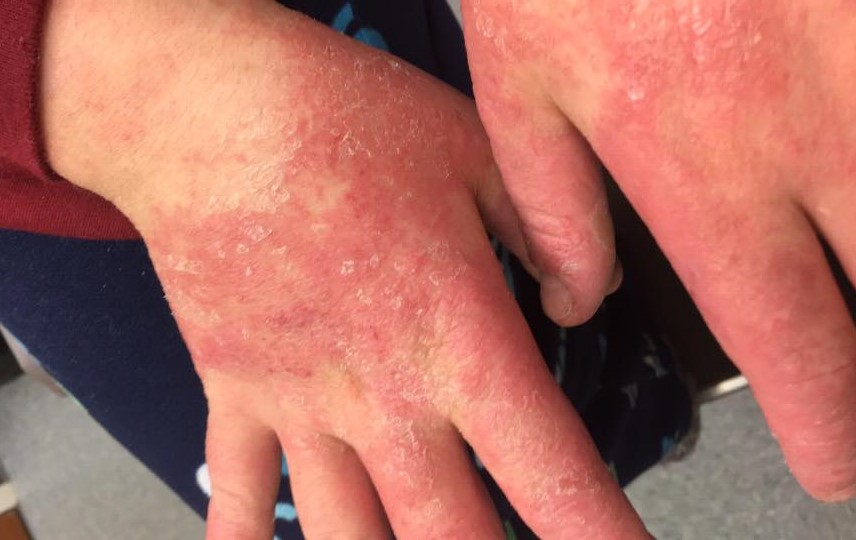
What are the common signs and symptoms of Eczema?
There are some symptoms which are common to all types of eczema.
• Dry scaly skin
• Redness and inflammation
• Itching – This can be intense. Usually it is more severe at night
Eczema is also referred to as ‘The itch that rashes’, because you may start your rash initially with itching. Your rash may develop or worsen with itching.
The other symptoms are;
• Chronic and persistent or repeatedly occurring symptoms
• The location of the rash is characteristic which is typical of eczema – commonly hands, wrists, inside elbows and knees, feet, ankles, upper chest and eye lids
• Dry and sensitive skin
• Associated oozing and crusting especially in wet eczema
• Swelling of lesions due to edema and inflammation
• Habitual scratching making the skin lesions thick and leathery
• Dark and discolored patches on skin
Why does your Eczema itch?



Itching is a symptom that almost all patients with eczema experience. It is usually ongoing day and night. Itching is the worst symptom according to most individuals. It can be so intense and may never go away.
Eczema flares can be frequently triggered by the ‘Itch –scratch cycle’. As itching leads to scratching, it can result in release of inflammatory mediators that develop the eczema and make your skin further dry. Eczema flares and dry skin may lead to more itching and the cycle continues.
Itching may occur due to many reasons, such as;
• Defective skin barrier in eczema
• External triggers
• Human nature – how you feel the itch and how well you can control the urge to scratch
• Sweating and perspiration induce itching and aggravate your eczema
Itching is a complex symptom in eczema and it is related to both physical and psychological causes. Many patients with eczema claim that it is impossible to resist the urge to scratch, when told to do so.
Does Eczema run in families?
Eczema can run in families. It is an atopic condition which may associate with other atopic conditions like Hay fever (Allergic rhinitis), allergic conjunctivitis or bronchial asthma. Genetic inheritance of allergic conditions is known as atopy. Atopy is linked with increased immune response to common allergens like inhaled allergens or certain foods.
Usually you may find a family history of one or more of these conditions suffered by a family member or a close relative.
What are the causes of Eczema?
The exact cause of eczema is unknown. Following factors may play a role;
• Your genes
• Immune system dysfunction
• If you have dry skin
• Factors that make your skin dry and sensitive to infection and irritants
Eczema occurs when the natural barrier of your skin is weakened. When this happens your skin is unable to protect you against various allergens and irritants. Eczema may be caused by a combination of factors.
There are certain factors which can trigger your eczema, such as;
• Irritants -wool, soap, detergents
• Allergens –Inhaled allergens like pollen, dust mites and ingested allergens like certain foods
• Heat and sweating
• Emotional stress
Can you manage your eczema?
You can try these remedies at home to control eczema and to prevent getting flares.
• Avoid scratching – Scratching worsens your eczema. Cover the itchy areas if you find it difficult to avoid scratching. Covering your rash with a bandage will not only prevent scratching, but will protect your skin too.
Trim the nails of children with eczema, to reduce the skin damage by scratching. Get them to wear gloves or anti-scratch mittens to prevent unintentional scratching especially at night.
• Use a mild, fragrance free soap when washing your skin. Pat dry with a soft towel. Do not wipe hard or rub your skin. Avoid strong soaps and detergents as they can worsen your eczema.
• Warm baths – Sprinkle your bath water with colloidal oat meal or baking soda. Soak your body for 15 minutes and pat dry.
• Moisturize your skin well and keep it hydrated – Use a good emollient regularly to moisturize your skin. Choose one which is alcohol and paraben free with minimal fragrance. Look for ingredients such as aqueous cream, Dimethicone, glycerol, Argon oil, Shea butter, cocoa butter and Lanolin oil when selecting a moisturizer. Choose an emollient that is suitable for your skin type.
• Apply your moisturizer after a bath when the skin is still damp. Damp skin absorbs and locks in the moisture well.
• Identify and avoid the triggers that is known to worsen your eczema.
Ex: Certain food items, Pollen, dust, excessive sweating and heat, strong soaps and detergents.
Identify them early and avoid. Avoid wool and tight, scratchy or rough clothing. Wear cooling clothes with smooth texture to minimize your skin irritation. When you are going out in hot weather or during your work outs, wear appropriate clothing to prevent excessive sweating.
• Manage your stress – practice relaxation techniques, yoga and meditation. Try to get quality sleep. Poor sleep can worsen your stress and make you less functional during day time
• Eat a balanced, healthy diet and void food triggers.
Are there any over the counter (OTC) products which you can use for Eczema?



OTC creams such as Hydrocortisone can be applied topically, which is a mild steroid.
Antihistamines like Cetirizine (Zyrtec),Loratadine (Alavert, Claritin),Fexofenadine (Allegra),Diphenhydramine (Benadryl) or Chlorpheniramine which are available over the counter can be used to reduce your itching. Make sure that the dose and the frequency of administration is correct when using any OTC medication.
Above home remedies and self- care measures can control your rash, relieve your itching and prevent new out breaks of eczema to a certain extent.
When should you seek help?
If your itching or rash doesn’t go away on its own or with home remedies you use or if it interferes with your day to day life or disturbs your sleep, it is time to see your doctor or a dermatologist. Look for any signs of infection such as red streaks or pus or even fever associated with your eczema.
Until you meet a dermatologist maintain a diary, so that it may be helpful to your doctor to identify what triggers your eczema. You can include;
1. Your diet – anything different you consumed
2. The skin products, make up and soaps you use
3. If you come in to contact with chemicals, detergents and other irritants
4. Activities you do – walk or jog outside where there is pollen or dust, swimming in chlorinated pools
5. Your bathing or showering patterns
6. Whether you are under stress
This diary will also help you to notice any connections between your eczema flare up and your activities, so that you can avoid such activities.
How will your doctor treat your eczema?
After taking the history and examination of your skin, your doctor will diagnose eczema clinically. Lab tests are usually not needed for diagnosis. Sometimes your doctor may perform a patch test to exclude skin conditions such as contact dermatitis.
Your doctor may have to try numerous treatments for months or even years until your eczema gets controlled. However, even after successful control you may get a sudden flare. Your doctor will advise you on how to identify and avoid triggers of eczema in order to prevent a flare.
You already know that regular moisturizing control your eczema. However, moisturizing per se is not adequate for effective control.
Your doctor will suggest some of the following treatments to control your eczema:
Best suitable emollient to moisturize your skin – If your skin is very dry, your doctor will prescribe an ointment. Ointments are very effective in keeping moisture of your skin. As ointments contain the most oil, they are greasy. A cream or a lotion will be adequate for less dry skin. Moisturizing should be done twice a day. A cream is more suitable to apply during day time. Since ointments are greasier you may apply them at night. Creams can sting more than ointments.
These prescribed creams or ointments not only treat your eczema, but also control your itching. They will improve your rash by repairing the damaged skin.
Some of the prescribed creams and ointments are;
Corticosteroid creams or ointments – After moisturizing your skin, apply a thin layer on the eczematous lesions. Your doctor will direct you regarding the frequency of application. It may be once or twice a day. Corticosteroids control inflammation therefore, redness of your skin and swelling will reduce.
Example:
Hydrocortisone – for lesions in your face, neck and other sensitive regions
Betamethasone – more potent steroid
Mometasone – effective corticosteroid with less side effects
Clobetasol – used for eczema on hands and feet, thick lesions
Moisturize first before applying the medicated creams, as it will help better penetration of your skin. Once the initial lesions are controlled, you can use topical corticosteroids less frequently, to prevent a flare. Do not overuse corticosteroids as they can lead tothinning of your skin.
• Calcineurin inhibitors –
Example:
Tacrolimus (protopic),
Pimecrolimus (Elidel)
Calcineurin inhibitors act by affecting your immune response. They are useful to treat eczema in sensitive areas and for lesions which do not respond to other treatments. After moisturizing your skin, apply as directed by your doctor. Avoid strong sun light when using calcineurin inhibitors. It is safe to use them in anyone above the age of 2 years.
For severe eczema your doctor may prescribe oral medications to fight inflammation and to control your symptoms.
• Oral corticosteroids – If your eczema is severe, your doctor will prescribe oral corticosteroids.
Ex: a course of oral prednisolone
Although they are effective, they cannot be used for long periods because of the potential side effects like osteoporosis and high blood pressure that can be serious.
• Medications to fight infection – If your eczema is associated with a bacterial infection an antibiotic cream will be added. If your infection is severe with pus discharge and fever, a short course of oral antibiotics will be prescribed.
• Antihistamines – Ex: Cetirizine (Zyrtec), Fexofenadine (Allegra), diphenhydramine
Antihistaminesare prescribed to control itching. Anti-itch medications may cause drowsiness. Therefore, use them before you go to bed.
• Dupilumab (Dupixent) – This is a new option for treating severe Eczema.
Dupilumabis an injectable biologic (monoclonal antibody) that is recently approved by the FDA. It is used in people with severe eczema who do not respond well to other medications. Dupilumab is an expensive drug. It is safe when used as directed. More studies are needed to identify the benefits of this medication.
Following therapies can be combined with the medications;
• Wet wraps – The affected region is wrapped with emollients, corticosteroids and wet bandages. This is shown to be effective in those with severe eczema. Since wet wrapping can be too intensive to do at home for patients with wide spread eczema, they are done at hospital setting. This requires good nursing care and expertise. However, if you are competent enough, you may do wet wrapping at home once you learn the proper technique.
• Light therapy – Phototherapy with artificial Ultra violet Alight (UVA) or narrow band ultra violet B light (NB- UVB) can be used alone or in combination with other treatments. You may try exposing your skin to natural sun light as light therapy but in controlled amounts.
Light therapy is beneficial in patients who do not respond to topical treatments or for those who get frequent flares.
• Dietary modifications – Certain dietary changes will be suggested by your doctor if your history suggests food triggers. Foods like cow’s milk, eggs, soy can trigger symptoms or lead to flares. If your doctor suspects a food allergy, you may be referred to a dietician to modify your diet.
• Behavior modification and other relaxation techniques –to keep your stress under control and to help those with habitual scratching.
• Counselling – Talk to your therapist or a counsellor for emotional support if you suffer from persistent eczema.
Eczema may be stressful especially for adolescents and young adults. It can disturb your sleep and disrupt your day to day routines. Long standing eczema may even lead to depression in some patients. Family members of patients with eczema can also face various emotional, social and financial difficulties. Never fight eczema alone. You can seek emotional support from support groups, counsellors, family and friends.
Take home message….
Eczema can be persistent. You may need various medications along with self- care measures for a long time to get it under control. Even after successful treatment, eczema can recur.
References:
https://www.mayoclinic.org/diseases-conditions/atopic-dermatitis-eczema/symptoms-causes/syc-20353273
https://www.mayoclinic.org/diseases-conditions/atopic-dermatitis-eczema/diagnosis-treatment/drc-20353279
https://www.nhs.uk/conditions/atopic-eczema/
https://nationaleczema.org/eczema/
GET IN CONTROL OF YOUR ECZEMA
Use our AI tool to check the severity of Eczema and keep track of your Eczema progress.