Psoriasis Symptoms, Types, Causes, Diagnosis & Treatment
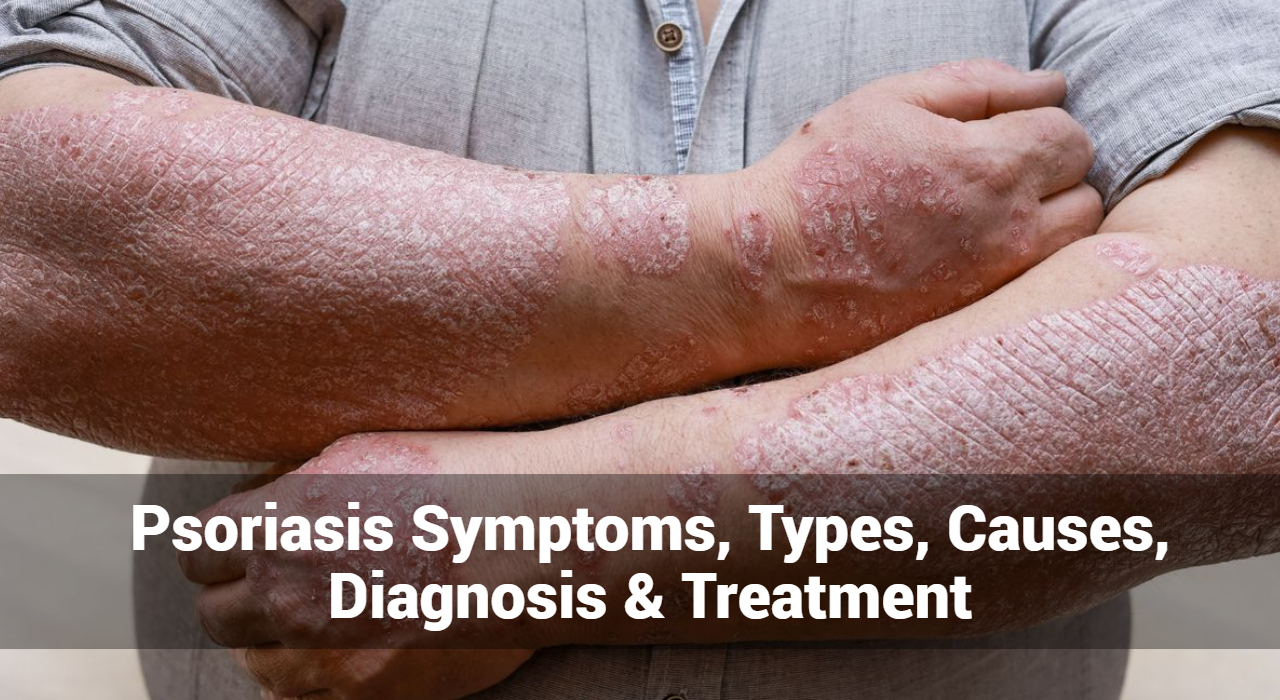
Psoriasis is a chronic autoimmune condition that affects the skin, causing red, scaly patches and discomfort for millions of people worldwide. Understanding the symptoms of psoriasis is crucial for early detection and effective management of the condition. In this guide, we’ll explore the common symptoms, types, causes, diagnosis, and treatment options for psoriasis.
Common Symptoms of Psoriasis:
- Red, Raised Patches: One of the hallmark symptoms of psoriasis is the presence of red, raised patches of skin, often covered with silvery-white scales. These patches, known as plaques, can appear anywhere on the body but are commonly found on the scalp, elbows, knees, and lower back.
- Itching and Discomfort: Psoriasis plaques can be itchy, tender, or sore, causing discomfort and irritation for affected individuals. Scratching the affected areas may worsen symptoms and lead to skin damage or infection.
- Thickened or Pitted Nails: In some cases, psoriasis can affect the nails, causing changes such as thickening, pitting (small dents or depressions), or separation of the nail from the nail bed. Nail psoriasis can be painful and may impact the appearance and function of the nails.
- Joint Pain and Swelling: Psoriasis is associated with a type of arthritis called psoriatic arthritis, which can cause joint pain, stiffness, and swelling, particularly in the fingers, toes, wrists, ankles, and lower back. Psoriatic arthritis can develop in individuals with psoriasis, leading to additional complications.
- Scalp Psoriasis: Psoriasis can also affect the scalp, causing red, scaly patches and flaking skin. Scalp psoriasis may be mistaken for dandruff but tends to be more persistent and difficult to treat.
What Are The Types of Psoriasis?
Psoriasis is a chronic autoimmune condition that affects millions of people worldwide, characterized by the rapid growth of skin cells, resulting in red, scaly patches and discomfort. While plaque psoriasis is the most common form, several other types of psoriasis exist, each with its unique characteristics and symptoms. Understanding the different types of psoriasis is crucial for accurate diagnosis and effective management. In this article, we’ll explore the various types of psoriasis, their symptoms, and treatment approaches.
1. Plaque Psoriasis: Plaque psoriasis, also known as psoriasis vulgaris, is the most common form of psoriasis, accounting for approximately 80% of cases. It presents as raised, red patches of skin covered with silvery-white scales, known as plaques. These plaques can appear anywhere on the body, but they commonly affect the scalp, elbows, knees, and lower back. Plaque psoriasis can be itchy and uncomfortable, and scratching the affected areas may cause bleeding or irritation.
2. Guttate Psoriasis: Guttate psoriasis is characterized by small, red spots or lesions scattered across the body, resembling droplets or tears. This type of psoriasis often develops suddenly, particularly in children and young adults, and is commonly triggered by bacterial infections such as streptococcal throat infections. Guttate psoriasis may resolve on its own or develop into other forms of psoriasis over time.
3. Inverse Psoriasis: Inverse psoriasis affects skin folds and areas of friction, such as the armpits, groin, under the breasts, and around the genitals. Unlike plaque psoriasis, which presents as raised plaques, inverse psoriasis appears as smooth, red patches of irritated skin. It may be exacerbated by sweating and friction and can cause discomfort or pain due to its location in sensitive areas.
4. Pustular Psoriasis: Pustular psoriasis is characterized by the presence of pus-filled blisters surrounded by red, inflamed skin. These blisters, known as pustules, can be localized or widespread and may appear on the hands, feet, or other parts of the body. Pustular psoriasis can be painful and may be accompanied by fever, chills, or other systemic symptoms. There are several subtypes of pustular psoriasis, including generalized pustular psoriasis and palmoplantar pustulosis.
5. Erythrodermic Psoriasis: Erythrodermic psoriasis is the least common but most severe form of psoriasis, characterized by widespread redness, scaling, and inflammation of the skin. It can cover the entire body surface and may be accompanied by intense itching, burning, or pain. Erythrodermic psoriasis is a medical emergency and requires immediate medical attention due to the risk of complications such as dehydration, infection, and changes in body temperature.
6. Nail Psoriasis: Nail psoriasis affects the nails, causing changes in their appearance and texture. Common symptoms include pitting (small dents or depressions), discoloration, thickening, crumbling, or separation of the nail from the nail bed. Nail psoriasis can be painful and may impact the appearance and function of the nails, leading to difficulties with activities of daily living.
Treatment Approaches: Treatment for psoriasis varies depending on the type, severity, and individual characteristics of the condition. It may include topical treatments such as corticosteroids, vitamin D analogs, and retinoids, phototherapy (light therapy), systemic medications such as methotrexate or biologic agents, and lifestyle modifications. Additionally, targeted therapies and alternative treatments may be used to manage specific symptoms or complications associated with psoriasis.
Psoriasis is a complex and multifaceted condition with various types and presentations. By understanding the different types of psoriasis and their unique characteristics, individuals can better recognize symptoms, seek appropriate medical care, and develop personalized treatment plans with their healthcare providers. If you or a loved one is experiencing symptoms of psoriasis, consult with a dermatologist or healthcare professional for an accurate diagnosis and comprehensive treatment approach tailored to your needs.
Causes and Triggers of Psoriasis:
The exact cause of psoriasis is not fully understood, but it is believed to involve a combination of genetic, immune, and environmental factors. Common triggers for psoriasis flare-ups include:
- Stress: Emotional stress or trauma can exacerbate psoriasis symptoms or trigger flare-ups in some individuals.
- Infections: Bacterial or viral infections, particularly streptococcal infections, can trigger guttate psoriasis or exacerbate existing psoriasis symptoms.
- Injury to the Skin: Trauma or injury to the skin, such as cuts, burns, or insect bites, can trigger the development of psoriasis lesions (known as the Koebner phenomenon).
- Certain Medications: Some medications, including beta-blockers, lithium, antimalarial drugs, and corticosteroids, can exacerbate or trigger psoriasis symptoms in susceptible individuals.
- Smoking and Alcohol: Smoking and excessive alcohol consumption have been linked to an increased risk of developing psoriasis and may worsen existing symptoms.
Track and Manage your Eczema treatment using a comprehensive Eczema App
Download Eczemaless now
What Part of My Body will Psoriasis Affect?
Psoriasis can affect various parts of the body, including:
- Skin: The most common site of psoriasis is the skin. Psoriasis lesions, known as plaques, can appear on any part of the body, but they often develop on the elbows, knees, scalp, lower back, and buttocks. Other areas commonly affected include the palms of the hands, soles of the feet, nails, and face.
- Scalp: Scalp psoriasis is common and can cause red, scaly patches and flaking skin on the scalp. It may extend beyond the hairline onto the forehead, neck, and ears.
- Nails: Psoriasis can affect the nails, causing changes in their appearance and texture. Symptoms may include pitting (small dents or depressions), discoloration, thickening, crumbling, or separation of the nail from the nail bed.
- Joints: Psoriasis is associated with a type of arthritis called psoriatic arthritis, which affects the joints. Psoriatic arthritis can cause joint pain, stiffness, and swelling, particularly in the fingers, toes, wrists, ankles, and lower back.
- Skin Folds: Inverse psoriasis affects skin folds and areas of friction, such as the armpits, groin, under the breasts, and around the genitals. It appears as smooth, red patches of irritated skin.
- Face: While less common, psoriasis can affect the face, causing redness, scaling, and discomfort. It may involve the eyebrows, eyelids, nasolabial folds (the creases that run from the sides of the nose to the corners of the mouth), and ears.
- Genital Area: Psoriasis can also affect the genital area, causing red, scaly patches and discomfort. It may be particularly challenging to manage in this sensitive area.
Psoriasis can vary widely in its presentation and severity from person to person. Some individuals may have mild symptoms that only affect small areas of the body, while others may experience more extensive involvement and complications. It’s essential to work closely with a healthcare provider, such as a dermatologist, to develop a personalized treatment plan tailored to your specific needs and symptoms.
How is Psoriasis Diagnosed?
Psoriasis is typically diagnosed based on a combination of clinical evaluation, physical examination, and sometimes additional tests. Here’s how psoriasis is diagnosed:
- Medical History: Your healthcare provider will begin by taking a detailed medical history, including information about your symptoms, any previous skin conditions or treatments, family history of psoriasis or other autoimmune disorders, and any potential triggers or exacerbating factors.
- Physical Examination: During a physical examination, your healthcare provider will carefully inspect your skin, nails, and scalp for characteristic signs of psoriasis, such as red, raised patches covered with silvery-white scales (plaque psoriasis), pitting or discoloration of the nails, or redness and scaling on the scalp.
- Skin Biopsy: In some cases, a skin biopsy may be performed to confirm the diagnosis of psoriasis and rule out other skin conditions with similar symptoms. During a skin biopsy, a small sample of skin tissue is taken from a psoriatic lesion and examined under a microscope by a dermatopathologist.
- Differential Diagnosis: Your healthcare provider will also consider other skin conditions that may resemble psoriasis, such as eczema, seborrheic dermatitis, pityriasis rosea, lichen planus, or fungal infections. Differential diagnosis may be challenging, as some skin conditions may coexist with or mimic psoriasis.
- Evaluation for Psoriatic Arthritis: If you have symptoms suggestive of psoriatic arthritis, such as joint pain, stiffness, or swelling, your healthcare provider may perform additional assessments, including a physical examination of the joints, imaging studies (such as X-rays or ultrasound), or blood tests to evaluate inflammation and immune function.
- Additional Tests: In some cases, additional tests may be ordered to assess the severity of psoriasis or monitor its impact on other organ systems. These may include blood tests to evaluate levels of inflammatory markers, liver function tests (especially if systemic medications are being considered), or imaging studies to evaluate joint involvement in psoriatic arthritis.
Overall, the diagnosis of psoriasis is based on a combination of clinical findings, physical examination, and sometimes additional tests or procedures. It’s essential to consult with a dermatologist or healthcare provider for an accurate diagnosis and appropriate management of psoriasis and any associated symptoms or complications. Early diagnosis and treatment can help control symptoms, prevent complications, and improve quality of life for individuals living with psoriasis.
What Are The Treatment Options for Psoriasis?
While there is no cure for psoriasis, several treatment options are available to help manage symptoms and improve quality of life:
- Topical Treatments: These include corticosteroids, vitamin D analogs, retinoids, coal tar preparations, and moisturizers applied directly to the skin to reduce inflammation and scaling.
- Phototherapy (Light Therapy): Phototherapy involves exposing the skin to ultraviolet (UV) light under medical supervision, which can help slow the growth of skin cells and reduce inflammation.
- Systemic Medications: For moderate to severe psoriasis, oral or injectable medications may be prescribed to suppress the immune system and reduce inflammation. These include methotrexate, cyclosporine, acitretin, and biologic agents.
- Lifestyle Modifications: Lifestyle changes such as stress reduction, maintaining a healthy weight, quitting smoking, and limiting alcohol consumption may help improve psoriasis symptoms and overall health.
- Alternative Therapies: Some individuals find relief from psoriasis symptoms through alternative therapies such as acupuncture, meditation, dietary supplements, and herbal remedies. However, it’s essential to consult with a healthcare professional before trying any alternative treatments.
Conclusion:
Psoriasis is a chronic autoimmune condition that affects the skin, nails, and joints, causing red, scaly patches, discomfort, and emotional distress for affected individuals. By understanding the symptoms, types, causes, diagnosis, and treatment options for psoriasis, individuals can better manage the condition and improve their quality of life. If you or a loved one is experiencing symptoms of psoriasis, consult with a dermatologist or healthcare provider for an accurate diagnosis and personalized treatment plan.


Use our AI tool to check the severity of Eczema and keep track of your Eczema progress
Recent Posts
- What Are Cherry Angiomas? It’s Causes, Symptoms & How To Treat
- Adult Acne: Types, Causes, Symptoms, Treatment & Prevention
- How to Relieve Winter Itch: Causes, Symptoms, and Treatment
- What Is Kaposi Sarcoma? It’s Symptoms, Causes & Treatment
- What Is Erythrasma: It’s Symptoms, Causes, And How To Treat


